【文献名】
David T. Liss, Jessica Chubak, Melissa L. Anderson, Kathleen W. Saunders, Leah Tuzzio, and Robert J. Reid
Patient-Reported Care Coordination: Associations With Primary Care Continuity and Specialty Care Use
Ann Fam Med 2011 9: 323-329.
【要約】
<Purpose>
Care coordination is increasingly recognized as a necessary element of high-quality, patient-centered care. This study investigated following.
1. The association between care coordination and continuity of primary care.
2. Differences in this association by level of specialty care use
<Methods>
Design : Cross-sectional study
Setting : Group Health, an integrated health care delivery system in Washington State and Idaho
Data collection : During March through September 2008, data were collected from questionnaires mailed to Group Health members who were eligible to enroll.
Participants: Eligible patients were aged 65 years or older, received care at a Group Health clinic in King County or Pierce County in western Washington State, and had at least 1 of the following chronic conditions: diabetes, coronary artery disease (CAD), or congestive heart failure (CHF).
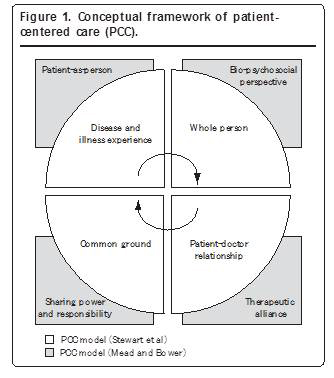
Coordination measure: The short form of the Ambulatory Care Experiences Survey (Figure1.)
Continuity measure: Primary care visit concentration.
Analysis: Linear regression was used to estimate the association between coordination and continuity, controlling for potential confounders and clustering within clinicians.
To determine whether the association between care coordination and continuity was modified by level of specialty use, an indicator for high specialty care use (10 or more specialist visits during the 1-year study period) and an interaction between high specialty care use and care continuity were included in the model.
<Results>
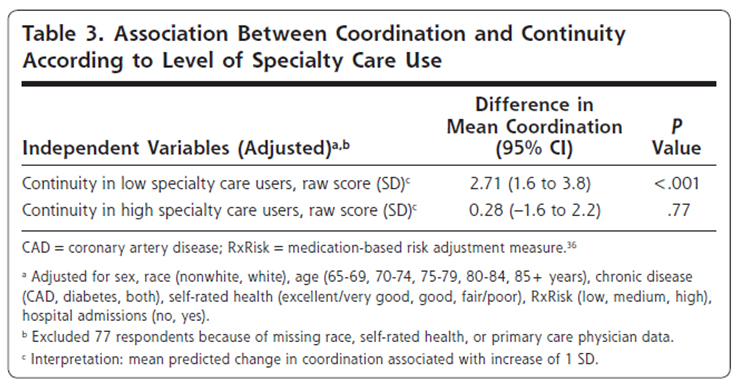
Among low specialty care users, an increase of 1 standard deviation in continuity of care was associated with an increase of 2.71 in coordination (P <.001, Table 3).
Among respondents with
high specialty care use, however, the model showed no association between continuity and reported coordination(P = .77).
<Conclusion> High use of specialty care may strain the ability of primary care clinicians to coordinate care effectively. Future studies should investigate care coordination interventions that allow for appropriate specialty care referrals without diminishing the ability of primary care physicians to manage overall patient care.
【開催日】
2011年8月31日