―文献名―
Mark H. Ebell, et al. Top 20 POEMs of the Past 20 Years: A Survey of Practice-Changing Research for Family Physicians. ANNALS OF FAMILY MEDICINE. 2018; VOL. 16, NO. 5 SEPTEMBER/OCTOBER: p436-439.
―要約―
1994年に、Slawson, Shaughnessy, and Bennettにより発表された論文によって、the key concepts of “information mastery”が確立された。従来のevidence-based practiceでは、研究のinternal validityの評価が重要視され、relevanceやapplicationは置いていかれていた。Information masteryによってpatient-oriented outcomesに注目が集まった。relevant clinical questionについての研究で、patient-oriented outcomesを出してpracticeを変えうるような論文は、POEM(patient-oriented evidence that matters)と呼ばれるようになった。
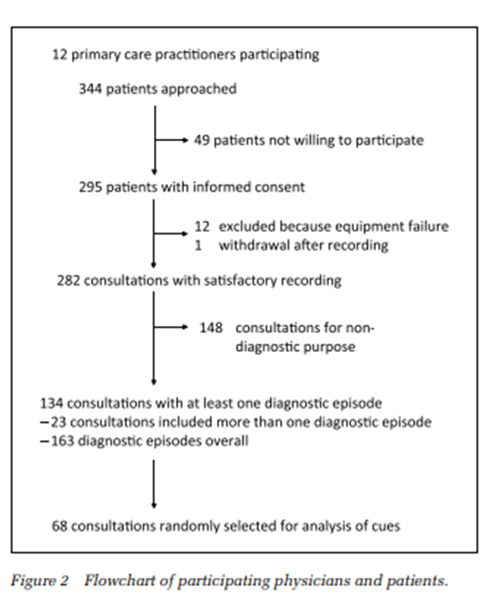
1998年に、筆者らはPOEMの定義に当てはまる論文を同定するために毎月100以上のclinical medical journals を集めたsystematic reviewを始めた。それぞれの論文は、primary care expertによってフォーマットに従って要約され、簡潔なbottom-line recommendation for practiceを提供した。それらはEssential Evidence Plusの購読者にメールされたりAFPに掲載されたりポッドキャストで配信されたりした。1998〜2017の20年間で、5,664のPOEMs (mean=283/y, range=230-368)が集まった。20週年を記念して、各年のPOEMsを選んだ。
They can be broadly divided into 3 groups:
(1) POEMs that recommend a novel, effective intervention,
(2) those that recommend abandoning an ineffective practice, and
(3) those that recommend abandoning a potentially harmful practice.
We observed greater challenges in choosing the best POEMs in recent years, largely because it is difficult to know whether a 3-year-old study will withstand the test of time and the rigors of replication in real-world settings. This judgment is even more difficult because of the increasing amount of industry-sponsored research published in journals and the relatively small amount of public funding for research to support the study of real-world problems in real-world settings.
It would be difficult for any clinician in any specialty or discipline to read all of the journals publishing studies of potential importance, not to mention critically evaluate the validity of individual relevant articles. Clinicians regularly reading POEMs can confidently change practice with the knowledge that they are using the very latest, most relevant, and valid information to provide for the very best care for their patients. The current POEMs are oriented toward primary care, including obstetrics and general hospitalists. We hope to encourage the development of POEMs for other specialties and disciplines in medicine, as well as such other health care disciplines as dentistry and veterinary medicine.
【開催日】2018年11月21日(水)